What Implant Patients Should Know About Sedation Options: A Clear Guide to Choices, Risks, and Recovery
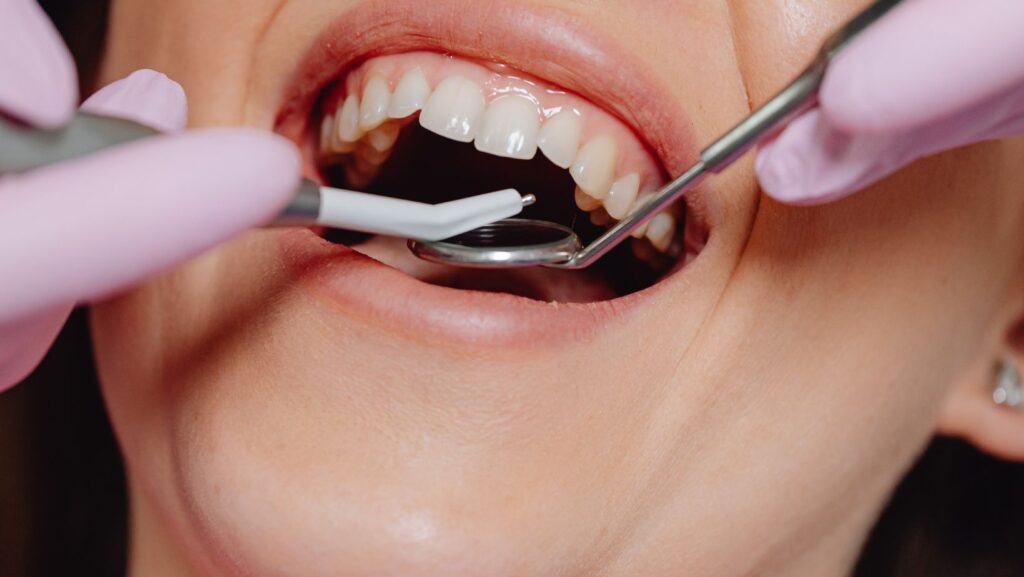
Getting a single tooth or multiple tooth dental implant can feel daunting, but you don’t have to face the procedure in fear. You have several safe sedation options—from local anesthesia and nitrous oxide to oral or IV sedation—that let your dental team match comfort and safety to your medical history and anxiety level.
This post explains how each option works, who benefits most from each level of sedation, and how to prepare for the experience so you feel informed and in control. Expect clear guidance on choosing the right method and what will happen before, during, and after sedation so you can move forward with confidence.
Overview of Sedation Options for Implant Patients
You’ll learn which sedation methods are available, how they affect consciousness and memory, and which medical or procedural factors guide their use.
Types of Dental Sedation
Local anesthesia numbs only the implant site; you stay awake and responsive. Dentists typically use lidocaine or articaine injections; local alone often suffices for single implants or minor bone work.
Nitrous oxide (laughing gas) provides mild to moderate anxiolysis and wears off quickly. You’ll inhale it through a mask and remain conscious, often feeling calm with reduced awareness of time.
Oral sedation uses pills like diazepam or triazolam taken before the appointment. You’ll be drowsy and may have limited memory of the procedure; plan for a responsible adult to drive you home.
IV sedation (moderate to deep) is delivered through a vein and titrated by the provider. You’ll be very drowsy and may have partial or full amnesia; deeper IV sedation approaches general anesthesia but is typically used for longer or multiple implants.
General anesthesia renders you completely unconscious and requires an anesthesiologist or qualified provider. Providers reserve it for extensive reconstructive cases or patients who cannot tolerate lighter sedation.
Suitability for Dental Implant Procedures
Single straightforward implant in a healthy patient often needs only local anesthesia. Choose nitrous oxide or oral sedation if you have moderate anxiety but good medical status.
Multiple implants, extensive bone grafting, or long surgical times favor IV sedation for better airway control and patient comfort. Your medical history—cardiac disease, sleep apnea, liver impairment—directly affects which sedatives are safe.
Pediatric patients or those with special healthcare needs may require deeper sedation or general anesthesia; plan with specialists. Always disclose medications, alcohol use, and allergies so the dental team can select drugs and dosing safely.
Facility resources matter: office-based IV sedation requires monitoring equipment and trained staff. If your dentist lacks that setup, they should refer you to an oral surgeon or hospital-based team.
Benefits and Limitations
Local anesthesia is low risk and allows rapid recovery, but it won’t reduce anxiety for fearful patients. It’s best when pain control, not sedation, is the main goal.
Nitrous oxide offers quick onset and recovery with minimal equipment, yet provides only moderate relaxation and may not be adequate for long or complex surgeries. It’s safe for many patients but less effective if used alone for deep procedures.
Oral sedation is convenient and cost-effective, producing stronger anxiolysis and amnesia than nitrous oxide. Downsides include variable absorption, longer recovery, and interactions with other drugs—dosing must reflect age, weight, and comorbidities.
IV sedation gives precise control and deeper sedation for complex implant cases, improving surgeon access and patient comfort. It carries higher risks—airway compromise, deeper cardiovascular effects—and requires advanced monitoring and trained personnel.
General anesthesia eliminates awareness and movement but increases recovery time and systemic risk. Reserve it for cases where other methods are insufficient or contraindicated.
Choosing the Right Sedation Method
You’ll weigh procedure complexity, your anxiety level, and medical risks to choose a safe, comfortable sedation plan. Your dentist or specialist will match a sedation level to the number of implants, surgical time, and your health history.
Factors Affecting Sedation Selection
Consider procedure details first: single-tooth implants often need only local anesthesia, while full-arch restorations or bone grafts may justify IV sedation or deep sedation. Expect longer or more invasive surgeries to require higher sedation levels for patient comfort and immobility.
Assess your anxiety and past responses to dental care. If you panic during dental work or have a history of gagging or severe discomfort, oral sedatives or nitrous oxide may be appropriate for mild-to-moderate anxiety; IV sedation works better for severe anxiety. Also factor in recovery time: nitrous wears off within minutes, oral sedatives can take hours, and deeper IV or general sedation requires longer monitoring.
Medical History Considerations
Provide a complete medical history, including medications, sleep apnea, heart or lung conditions, and prior reactions to anesthesia. Certain drugs (benzodiazepines, opioids) interact with sedatives; your provider may change dosages or pause medications before surgery.
Height, weight, and airway anatomy matter for dosing and safety. Obesity and obstructive sleep apnea raise the risk of breathing problems with deeper sedation and may steer the team toward lighter sedation plus local anesthesia. Pregnancy, uncontrolled diabetes, recent heart attack, or severe liver disease often limit sedation choices and require coordination with your physician.
Consultation With Your Dental Professional
Bring a list of current medications, allergies, and past anesthesia experiences to your consultation. Expect the clinician to review risks, obtain informed consent, and explain pre-op instructions such as fasting, medication adjustments, and transportation plans.
Ask specific questions: “Which sedation level do you recommend for my implant type?” “Who will monitor my vitals and what equipment is used?” “What are expected recovery times and aftercare?” Confirm provider credentials—whether the sedation will be administered by your dentist, a trained anesthesiologist, or a certified sedation nurse—and ensure emergency protocols and monitoring (pulse oximetry, blood pressure, oxygen) are in place.
What to Expect Before, During, and After Sedation
You will receive specific instructions about eating, medications, transportation, and monitoring that match the sedation level chosen. Staff will explain what sensations to expect during the procedure and what activities to avoid afterward.
Preparation and Pre-Procedure Guidelines
Follow fasting instructions exactly: typically no solid food for 6–8 hours and clear liquids up to 2 hours before IV or general sedation. For nitrous oxide or light oral sedation, eating a light snack 2–3 hours before may be allowed; confirm with your provider.
Bring a list of current medications and allergies. Your clinician may advise continuing or pausing blood thinners, diabetes meds, or SSRIs—get written directions beforehand. Arrange a responsible adult to drive you home and stay with you for several hours if you receive moderate-to-deep sedation.
Wear loose, comfortable clothing and avoid jewelry, contacts, and heavy makeup. Expect a pre-op assessment: vitals, medical history review, and informed consent forms that describe risks and emergency plans.
The Sedation Experience
With local anesthesia only, you stay fully awake but comfortable; you’ll feel pressure, not sharp pain. Nitrous oxide (laughing gas) produces mild relaxation and rapid recovery—you remain cooperative and responsive.
Oral sedatives (e.g., a benzodiazepine) cause drowsiness and reduced anxiety; you may feel groggy and have limited memory of the procedure. IV sedation provides faster, adjustable depth; clinicians monitor oxygen, heart rate, and blood pressure continuously. General anesthesia renders you unconscious and requires an anesthetist for airway management and deeper monitoring.
Tell the team immediately about shortness of breath, chest pain, or severe nausea. Staff will document sedation dose, time, and monitoring records in your chart.
Recovery and Aftercare Instructions
Expect drowsiness, slowed reaction time, and possible short-term memory gaps for several hours after oral or IV sedation. Do not drive, sign legal documents, or operate machinery for 24 hours unless your clinician gives other instructions.
Follow written wound care: keep the implant site clean, use prescribed antibiotics or pain meds as directed, and avoid rinsing vigorously for 24 hours. Apply ice to reduce swelling during the first 24 hours and eat soft foods for several days.
Watch for red flags: uncontrolled bleeding, fever over 101°F (38.3°C), severe pain not relieved by medications, or persistent vomiting. Contact your clinic immediately if any of these occur or if you have breathing difficulties. Keep your follow-up appointment for stitch removal and progress assessment.

 Recognizing Abuse in Elder Care Facilities
Recognizing Abuse in Elder Care Facilities  What Actions Are Considered Domestic Violence?
What Actions Are Considered Domestic Violence?  A Comprehensive Guide to CPR Certification Requirements by State
A Comprehensive Guide to CPR Certification Requirements by State  Why Does Bacteria Affect My pH Levels?
Why Does Bacteria Affect My pH Levels?  Small Daily Fitness Habits That Transform Your Well-Being
Small Daily Fitness Habits That Transform Your Well-Being  Why 3-Wheel Mobility Scooters Are Ideal For Seniors?
Why 3-Wheel Mobility Scooters Are Ideal For Seniors?