Can You Sleep Through Dental Implant Surgery? What to Expect, Risks, and Anesthesia Options
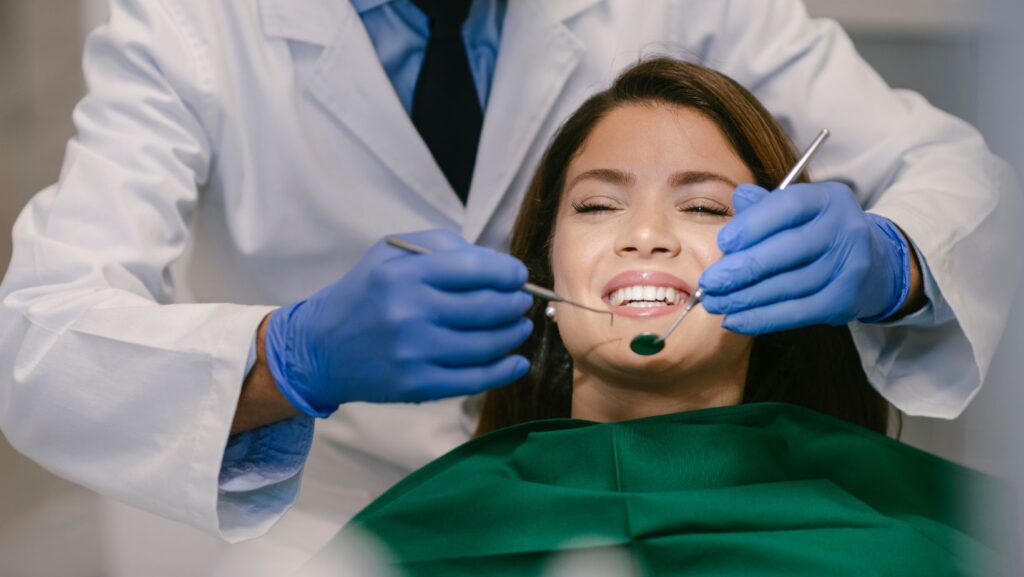
You can often have dental implant surgery without being fully unconscious—most procedures use local anesthesia, and many practices offer sedation options so you stay relaxed or lightly drowsy. If you want to sleep through the procedure, IV or deeper sedation is usually available, but your dentist or oral surgeon will recommend the safest option based on the complexity of your case and your medical history.
This article explains what happens during dental implant placement, exactly how different sedation levels feel, and what factors affect whether you can safely sleep through the operation. By the end, you’ll know which questions to ask your provider so you can plan the most comfortable, safe experience for your situation.
What to Expect During Dental Implant Surgery
You will learn the anesthesia choices, step-by-step actions your surgeon will take, and the comfort measures used before, during, and after the procedure. Expect clear instructions, brief waiting periods while anesthesia takes effect, and staff checking your vital signs.
Anesthesia Options Explained
You will typically receive one of three anesthesia approaches: local anesthesia, conscious (sedation) anesthesia, or general anesthesia. Local anesthesia numbs the surgical area; you stay awake and feel pressure but no sharp pain. Conscious sedation can be oral pill (e.g., triazolam), nitrous oxide, or IV sedation (e.g., midazolam or propofol); you remain responsive but deeply relaxed and may have limited memory of the procedure.
General anesthesia renders you fully unconscious and is reserved for complex cases, extensive grafting, or patients with severe anxiety or medical needs. The surgical team reviews your medical history and chooses the safest option; an anesthetist accompanies IV or general anesthesia cases. Expect fasting instructions and a post‑op recovery window for sedation to wear off.
Common Surgical Procedures
Most implant surgeries follow a predictable sequence: site preparation, implant placement, and closure. First, the surgeon makes a small incision in the gum to expose bone, then removes any damaged tooth fragments if present. Next, a pilot hole is drilled and gradually widened to the precise diameter and depth for the implant fixture; torque values are measured to confirm stability.
If you need a bone graft or sinus lift, that step occurs before or during implant placement; grafts can add 3–6 months to healing time. After the implant is seated, the surgeon places a healing cap or cover screw and closes the incision with sutures. Expect the procedure time to range from about 30 minutes for a single straightforward implant to several hours for multiple implants plus grafting.
Patient Comfort Measures
Your comfort starts before surgery with a clear preoperative plan and medications. You may receive a premedication for anxiety, a local anesthetic injection at the site, and intraoperative IV fluids if receiving sedation. The team monitors blood pressure, oxygen saturation, and heart rate throughout the procedure.
During surgery, the clinician uses gentle tissue handling, suction to keep the field clear, and breaks if you need adjustments in sedation or positioning. Afterward, the staff gives written and verbal aftercare instructions, pain‑control prescriptions (NSAIDs and/or short‑course opioids when indicated), and antibiotics if needed. You should arrange a responsible adult to drive you home when sedation or general anesthesia is used.
Can You Sleep Through Dental Implant Surgery?
You can be fully awake, deeply relaxed, or briefly unconscious during implant placement depending on the anesthesia used. Each option affects your awareness, memory, and recovery needs in different ways.
Types of Sedation and Their Effects
Local anesthesia numbs only the implant site so you remain conscious but feel no pain. You will respond to commands and have normal breathing; many patients feel pressure but not sharp pain.
Oral sedatives are pills (e.g., a benzodiazepine) taken before the procedure that make you drowsy and amnesic. You remain responsive but may not recall parts of the surgery. Breathing and reflexes are typically intact, but you should not drive afterward.
IV sedation ranges from moderate (you’re relaxed and sleepy but arousable) to deep (barely responsive). Dosing is titrated by the clinician; deeper levels may require airway monitoring and supplemental oxygen.
General anesthesia renders you fully unconscious and unresponsive. Providers secure the airway and deliver anesthetic gases or IV agents. This option is less common for straightforward implants and usually reserved for long, complex cases or patients with severe anxiety.
Choosing the Right Sedation for You
Discuss your medical history, anxiety level, and the complexity of the implant with your dentist or oral surgeon. They will consider conditions like sleep apnea, heart or lung disease, medication interactions, and pregnancy when recommending sedation.
If you have mild anxiety and a short, single-implant procedure, local anesthesia with or without oral sedation often suffices. For multiple implants, bone grafting, or strong claustrophobia, IV sedation or general anesthesia may be safer and more comfortable.
Ask who will monitor you, what monitoring devices will be used (pulse oximeter, blood pressure cuff, capnography), and where recovery will occur. Confirm fasting instructions, medication adjustments, and whether you need a responsible adult to take you home.
Safety of Sleeping Through the Procedure
Sedation and general anesthesia have well-established safety protocols when administered by trained professionals. Clinics follow guidelines for monitoring vital signs, maintaining oxygenation, and having resuscitation equipment on hand.
Risks increase with deeper sedation, certain medical conditions, and inadequate monitoring. Tell your provider about all medications, supplements, and prior anesthesia reactions to reduce complications.
You should receive written pre-op instructions and post-op monitoring until awake and stable. A responsible adult should drive you home for any sedation beyond local anesthesia and stay with you for the first 24 hours if deep sedation or general anesthesia was used.
Recovery and Post-Operative Considerations
Expect a short period of grogginess, bleeding control, and targeted pain management immediately after the procedure. Sleep position, medication timing, and wound care all affect how quickly you return to normal activities.
Waking Up After Surgery
You will usually wake up in the recovery area within 15–60 minutes if you had IV sedation or general anesthesia. Staff monitor your oxygen levels, blood pressure, and responsiveness until you meet discharge criteria.
Drowsiness and lightheadedness are common for several hours; arrange a capable adult to drive you home and stay with you. Avoid standing quickly and don’t operate machinery for at least 24 hours.
Expect mild bleeding or oozing from the implant site for 12–24 hours. Bite on gauze as instructed and change it when saturated. If bleeding soaks through a gauze pad every 20–30 minutes despite pressure, contact your clinic.
Managing Pain and Discomfort
Follow the exact medication schedule your dentist prescribes; do not skip doses of prescribed analgesics during the first 48–72 hours. Over-the-counter ibuprofen (200–400 mg every 4–6 hours) often pairs well with acetaminophen for moderate pain unless contraindicated.
Apply an ice pack to the outside of your cheek for 15 minutes on, 15 minutes off during the first 24 hours to reduce swelling. Sleep with your head elevated to minimize edema and throbbing overnight.
Expect tenderness at the implant site and the surrounding tissues for 7–14 days. Use saltwater rinses starting 24 hours after surgery, and avoid vigorous spitting or swishing. If you develop severe pain, fever, increasing swelling, or pus, contact your provider immediately.
Short-Term Versus Long-Term Effects
Short-term effects include localized swelling, bruising, mild fever, and temporary changes in taste or numbness from local anesthetic. Most of these resolve within 1–2 weeks with proper care and hygiene.
Long-term considerations focus on osseointegration (bone fusing to the implant), which typically takes 3–6 months. During this period, avoid biting directly on the implant site and follow any dietary restrictions to prevent micromovement that can impair healing.
Monitor for signs of chronic problems such as persistent numbness, implant mobility, or recurrent infection. Schedule follow-up visits as recommended so your clinician can assess stability and plan for the prosthetic crown when osseointegration is adequate.

 Recognizing Abuse in Elder Care Facilities
Recognizing Abuse in Elder Care Facilities  What Actions Are Considered Domestic Violence?
What Actions Are Considered Domestic Violence?  A Comprehensive Guide to CPR Certification Requirements by State
A Comprehensive Guide to CPR Certification Requirements by State  Why Does Bacteria Affect My pH Levels?
Why Does Bacteria Affect My pH Levels?  Small Daily Fitness Habits That Transform Your Well-Being
Small Daily Fitness Habits That Transform Your Well-Being  Why 3-Wheel Mobility Scooters Are Ideal For Seniors?
Why 3-Wheel Mobility Scooters Are Ideal For Seniors?