Does Sedation Dentistry Reduce Implant Surgery Stress? Clear Benefits, Risks, and What to Expect
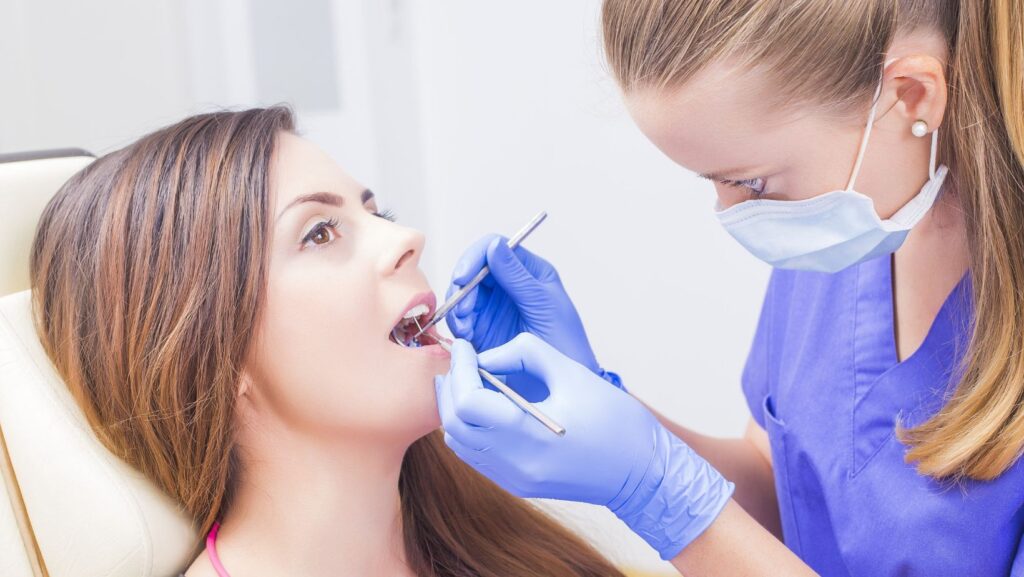
If the idea of implant surgery makes you anxious, sedation dentistry can greatly reduce stress by keeping you relaxed, comfortable, and pain-controlled throughout the procedure. Options such as nitrous oxide, oral medication, or IV sedation help manage both anxiety and physical discomfort, allowing the dental team to perform complex implant treatment more efficiently and safely.
This post explains how different sedation levels work, how each option affects awareness and recovery, and what safety considerations to review before treatment. By understanding the benefits and trade-offs, you can choose the level of comfort that best fits your needs. If you’re exploring comfort-focused care, learning more about oral sedation dentistry in Greenville, SC can help you discuss the right approach with your dental team before implant surgery.
Understanding Sedation Dentistry
Sedation dentistry controls anxiety, pain, and memory during implant surgery while keeping you safe and monitored. It ranges from mild relaxation to deeper sedation that blunts awareness, and the choice depends on your medical history, procedure complexity, and comfort goals.
Types of Sedation Used in Dentistry
Sedation options fall into four common categories: local anesthesia, nitrous oxide (laughing gas), oral conscious sedation, and IV (intravenous) sedation. Local anesthesia numbs the surgical site so you feel no pain but stay fully awake. Nitrous oxide provides mild to moderate relaxation, works quickly, and wears off fast—useful for anxiety without lengthy recovery.
Oral sedatives (usually benzodiazepines) produce moderate sedation; you’ll feel drowsy and may have limited memory of the procedure. IV sedation ranges from moderate to deep and allows the dentist or anesthesiologist to titrate drug levels for precise control. Equipment for monitoring heart rate, oxygen saturation, and blood pressure is standard with moderate-to-deep sedation. Discuss allergies, medications, and prior reactions with your provider to determine the safest option.
Candidates for Sedation in Dental Implant Procedures
You qualify for sedation if dental anxiety, a low pain threshold, a strong gag reflex, or a complex surgical plan would make cooperation difficult. Medical conditions—such as severe hypertension, obstructive sleep apnea, certain heart or lung diseases, and specific medication regimens—require tailored sedation plans or alternative approaches.
Age, BMI, and substance use also affect candidacy and monitoring needs. Pregnant patients typically avoid most sedatives. If you have multiple medical issues or take blood thinners, your dentist will consult your physician and may choose lighter sedation or hospital-based anesthesia. Prepare by sharing your full medical history, current medications, and past anesthesia experiences.
Overview of Dental Implant Surgery
Dental implant surgery commonly involves placing a titanium post into the jawbone to replace a missing tooth root. Procedures range from a single implant done in 30–60 minutes to multi-implant grafting that can take several hours and multiple visits. Bone grafts or sinus lifts add complexity and recovery time.
You’ll receive local anesthesia at a minimum; sedation is added for comfort, anxiety control, and to keep you still during delicate bone work. Postoperative instructions typically include pain control, antibiotics when indicated, and soft-food guidelines. Proper sedation helps you remain calm and still, which can improve surgical accuracy and reduce procedural stress.
Impact of Sedation Dentistry on Implant Surgery Stress
Sedation lowers the immediate emotional and physiological responses that make implant surgery feel threatening. It also helps you tolerate longer procedures and follow clinician instructions more easily, improving surgical precision and comfort.
How Sedation Reduces Patient Anxiety
Sedation reduces anxiety by altering your conscious awareness and lowering sympathetic nervous system activity. Minimal (nitrous oxide) and moderate (oral or IV benzodiazepines) sedation produce calmness, slower heart rate, and reduced subjective fear so you feel less tense before and during implant placement.
You remain responsive with moderate sedation, which lets the clinician give simple instructions while you stay relaxed. For longer or more complex implants, deeper IV sedation or monitored general anesthesia prevents movement and reduces recall, which many patients report as the key benefit.
Risks and monitoring matter: continuous oxygen, pulse, and blood pressure checks and trained staff reduce complications. Discuss medical history, medications, and fasting instructions with your provider to optimize safety and anxiolysis.
Mechanisms Behind Stress Reduction
Sedation works through pharmacologic and behavioral pathways to lower stress. Drugs such as benzodiazepines enhance GABA neurotransmission, which decreases neuronal excitability and reduces anxiety and memory formation related to the procedure.
Physiologic stress markers—heart rate, blood pressure, and cortisol—typically decline under appropriate sedation, which reduces the risk that acute stress will complicate anesthesia or surgical healing. Reduced muscle tension also makes local anesthesia and implant placement technically easier.
Behavioral mechanisms include increased patient cooperation and less need for sudden corrections during surgery. That smoother workflow minimizes surgical interruptions, which reduces procedural time and lowers cumulative stress for you and the surgical team.
Comparing Patient Experiences With and Without Sedation
With sedation, most patients report lower pain anticipation, less intraoperative movement, and little to no vivid memory of the procedure. You’re more likely to tolerate longer sessions—single-visit full-arch or multiple implant placements—without needing frequent breaks.
Without sedation, anxiety can raise heart rate and blood pressure, increase perceived pain, and make you more likely to move or request pauses. That can extend surgery time and complicate precise implant placement.
Clinicians balance benefits against individual risk factors. If you have severe dental phobia, medically controlled hypertension, or need complex, lengthy surgery, sedation often improves your experience and surgical conditions.
Considerations and Potential Risks
Understand common side effects, the safety steps your team should take during implant surgery, and what to do before the appointment to reduce complications and delays.
Possible Side Effects of Sedation
Sedation can cause nausea, dizziness, and prolonged drowsiness after the procedure. These effects vary by agent: oral benzodiazepines often produce residual grogginess for several hours, while IV sedatives can cause transient low blood pressure or slowed breathing.
Less common reactions include allergic responses, paradoxical agitation (more common with some benzodiazepines), and local injection-site bruising. If you take opioids, benzodiazepines, or certain antidepressants, drug interactions can increase respiratory depression risk. Tell your clinician about all prescriptions, OTC drugs, supplements, and recreational substances.
Monitor for difficulty breathing, chest pain, or severe confusion after sedation. Seek emergency care if these occur. Bring a responsible adult to drive you home and stay with you for the first 12–24 hours if heavy sedation was used.
Safety Precautions for Implant Procedures
Your dental team should perform a pre-procedure medical assessment that includes ASA (American Society of Anesthesiologists) classification, airway evaluation, and a review of cardiac, pulmonary, and hepatic history. Facilities should have pulse oximetry, capnography when available, oxygen, suction, and emergency airway equipment on hand.
Confirm that staff are trained in advanced cardiac life support (ACLS) or pediatric life support if needed, and that clear protocols exist for escalating to general anesthesia or hospital transfer. For lengthy or complex implant surgery, consider intraoperative monitoring of blood pressure, oxygen saturation, and end-tidal CO2.
Discuss sedation depth options—minimal, moderate, deep, or general—and choose the lowest effective level. If you have sleep apnea, severe obesity, or significant cardiopulmonary disease, the team may recommend hospital-based anesthesia for added safety.
Consultation and Preparation Guidelines
Provide a complete medical history, including previous reactions to anesthesia, smoking status, and alcohol use. Labs or medical clearance may be required if you have uncontrolled diabetes, cardiac stents, or anticoagulant therapy.
Follow pre-op fasting instructions precisely: typically no solid food for 6–8 hours and clear liquids until 2 hours before moderate sedation, unless your clinician advises otherwise. Stop or adjust blood thinners only under direct guidance from the prescriber and the dental surgeon to balance bleeding and thrombotic risk.
Arrange transportation and postoperative support. Ask the clinician to explain the chosen sedative, expected recovery timeline, potential interactions with your medications, and an explicit plan for managing complications, including whom to contact after hours.

 The Smart Patient’s Guide to Diagnostic Imaging: Ultrasound, X-Ray, and What to Expect
The Smart Patient’s Guide to Diagnostic Imaging: Ultrasound, X-Ray, and What to Expect  How Cannabinoids Can Help You Sleep Better
How Cannabinoids Can Help You Sleep Better  Exploring the Holistic Approach of Traditional Chinese Medicine: An Insight into
Bojin Therapy
Exploring the Holistic Approach of Traditional Chinese Medicine: An Insight into
Bojin Therapy  2026 Online Stores Guide for Purchasing CBD Gummies
2026 Online Stores Guide for Purchasing CBD Gummies  How Sleeping Position Quietly Determines Whether Lower Back Pain Improves or
Worsens Overnight
How Sleeping Position Quietly Determines Whether Lower Back Pain Improves or
Worsens Overnight  How to Build a Minimal Spring Wardrobe That Works All Season
How to Build a Minimal Spring Wardrobe That Works All Season